
Our Office
5909 South Congress Ave
Lake Worth, FL 33462
Existing Patients: (561) 967-6453
New Patients: (561) 203-0359
Emergency: (754) 800-1949
Fax: (561) 431-5866
Visit Us Online

At Horizon Palms Family Dentistry, our priority is protecting your long-term oral health while keeping you comfortable and informed. Tooth removal is never the first option we recommend, but there are clear situations where extraction is the safest, most predictable path to prevent ongoing pain, infection, or damage to neighboring teeth.
We approach every extraction with the same careful planning we apply to preventive and restorative care. That means a thorough review of your medical and dental history, targeted imaging when needed, and a clear discussion about what the procedure will involve and what to expect afterward.
Our team works to minimize anxiety and to tailor the experience to each patient—whether that means extra explanation, a calming chair-side presence, or discussing sedation options. The goal is to remove the source of trouble while preserving as much function and appearance as possible.
Primary (baby) teeth that are obstructing proper development
Sometimes a deciduous tooth refuses to loosen on schedule. If the root fails to resorb or the tooth becomes fused to the jawbone, it can block the arrival of the permanent tooth and cause alignment problems. Removing an over-retained baby tooth can help guide a healthier eruption pattern and avoid more complex orthodontic issues later.
Permanent teeth with irreversible damage from decay
When decay progresses beyond repair and the remaining structure can't reliably support a filling or crown, extraction may be the responsible choice. Leaving a severely compromised tooth in place can lead to persistent infection, pain, or deterioration of adjacent teeth and bone.
Teeth fractured below the gumline or badly broken
A deep crack or fracture that extends into the root often leaves insufficient healthy tooth to restore. In these cases, extraction prevents recurrent problems and sets the stage for replacement options that restore function and appearance.
Advanced periodontal disease compromising support
When gum disease is severe, the bone and soft tissues that anchor teeth can be lost. Teeth that have become loose or are contributing to infection and inflammation may need to be removed to halt the disease process and protect neighboring teeth.
Wisdom teeth that are impacted, painful, or damaging adjacent teeth
Third molars often do not have adequate space to erupt and can become impacted, partially erupted, or decay-prone. Removing problematic wisdom teeth can relieve discomfort, protect surrounding teeth, and reduce the risk of cysts or recurrent infections.
Extractions as part of orthodontic planning
Occasionally, removing one or more teeth is the right step to create space and allow orthodontic treatment to achieve a balanced, functional bite. In these situations, extractions are planned carefully with future alignment and facial proportions in mind.
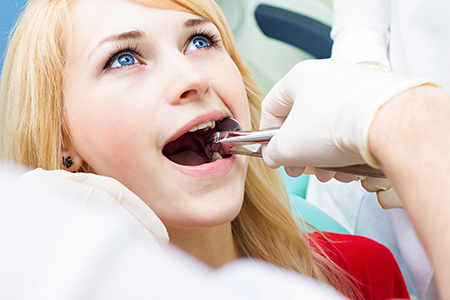
Before any procedure, we perform a comprehensive assessment to make sure extraction is the best course. This includes a review of your overall health, current medications, and any conditions that could affect healing. We also discuss your goals so treatment decisions align with your expectations for function and appearance.
Diagnostic imaging is an important part of the planning process. Clear radiographs help us evaluate root shape, position, and proximity to vital structures. This information determines whether a tooth is likely to be removed with simple instruments or will require a surgical approach.
If you have medical conditions that could complicate surgery—such as bleeding disorders, certain heart conditions, or immune system considerations—we coordinate care with your physician and make appropriate adjustments. For anxious patients, we explain sedation options and what to expect before, during, and after the appointment.
We also provide clear pre-operative instructions to reduce risk and promote smooth recovery. These directions cover medication guidance, eating and drinking recommendations, and any specific steps to take if you develop symptoms or illness before your scheduled visit.
A simple extraction is performed when a tooth is visible and can be loosened and removed with forceps after the area is numb. These procedures are typically quick and well-tolerated, with local anesthesia providing effective pain control.
A surgical extraction is used for teeth that are not easily accessible—such as broken roots, impacted teeth, or teeth with atypical root shapes. Surgical techniques may include a small incision in the gum and targeted removal of a bit of bone to allow safe tooth removal. These procedures can require careful post-operative monitoring and follow-up.
Whether a case is simple or surgical, we take steps to control pain and minimize healing time. Expect a thorough explanation of the planned approach, answers to your questions, and a personalized recovery plan when you leave the office.
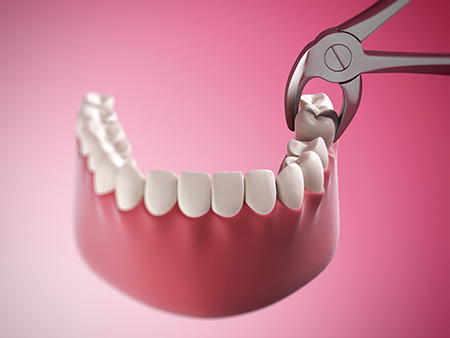
Care after an extraction has a major influence on how comfortably and quickly you heal. We give patients straightforward instructions to protect the extraction site, manage discomfort, and watch for signs of complications. Following these steps helps reduce swelling, prevent infection, and support the formation of a healthy blood clot.
Every patient is different, so we tailor post-op directions to the specifics of your procedure. We also schedule follow-up visits when appropriate, especially for surgical extractions or cases where stitches were placed, so we can monitor healing and address any concerns.
If you experience unusual symptoms—such as persistent heavy bleeding, fever, or severe pain that doesn’t respond to medication—contact the office promptly so we can evaluate the situation and recommend the next steps.
Maintaining gauze pressure
We place gauze over the site immediately after extraction; gentle, consistent pressure helps the socket clot. Change the gauze as instructed, and if bleeding persists more than a few hours or becomes heavy, reach out to the office.
Protect numb tissues
Until the anesthesia wears off, avoid chewing, hot liquids, or touching the area to prevent accidental biting of the lip, cheek, or tongue.
Medications and infection control
Antibiotics:
If prescribed, take the full course exactly as directed to reduce the risk of post-operative infection.
Pain management:
Start pain relief as recommended so discomfort is easier to control. Over-the-counter options or prescribed medications may be used according to instructions.
Protect the forming clot
Avoid rinsing vigorously, using straws, or smoking for several days. These actions can dislodge the clot and delay healing or cause painful complications.
Manage swelling
Apply an ice pack to the cheek in intermittent intervals during the first 24 hours to reduce inflammation and discomfort.
Avoid tobacco
Smoking and other tobacco use impair blood flow and healing; avoid them for at least a week after extraction to support the best possible recovery.
Choose gentle foods
Soft, lukewarm foods are advisable for the first several days. Steer clear of spicy or very hot items and limit alcohol and carbonated beverages while you heal.
Oral hygiene around the site
Keep the mouth clean by gently brushing other teeth and using a mild saltwater rinse after the initial 24 hours, taking care not to disturb the healing socket.
Follow-up care
Attend any scheduled appointments so we can remove stitches if needed and confirm that healing is progressing as expected.
If bleeding, pain, or swelling worsens, or if you notice an unusual taste or odor, contact the practice so we can advise you on next steps.
Removing a tooth often begins a conversation about what comes next. Leaving a gap can affect chewing, speech, and the alignment of neighboring teeth, so we discuss replacement options when appropriate and timing that makes sense for healing and long-term function.
Replacement choices include removable dentures, fixed bridges, and dental implants. Each option has distinct benefits related to stability, appearance, bone preservation, and maintenance. We explain how each solution works and which may best meet your needs based on the location of the missing tooth, oral health, and your goals.
When a dental implant is a candidate, we evaluate bone volume and overall health to determine suitability and timing. In many cases, preserving the jawbone and providing the most natural function and feel are key advantages of implant-supported restoration.
We combine clinical experience with individualized care, taking the time to explain procedures, answer questions, and ensure each patient leaves with a clear plan for recovery and future care. Our focus is on predictable outcomes and on preserving oral health for years to come.
Whether an extraction is routine or complex, our team uses modern techniques and thoughtful planning to reduce discomfort and promote efficient healing. We also coordinate with specialists when cases call for advanced surgical support to ensure the safest, most effective care.
If you would like to learn more about tooth extraction or how we approach replacement options, please contact us for more information and to schedule a consultation. We’ll review your situation and recommend a care plan tailored to your needs.
Extraction is recommended when a tooth is causing persistent pain, recurrent infection, or structural damage that cannot be reliably repaired. Common situations include severe decay that destroys most of the tooth, fractures that extend under the gumline, advanced periodontal disease, impacted wisdom teeth, and primary teeth that block proper eruption of permanent teeth. In some orthodontic plans, removal is indicated to create space for a healthy, functional bite. When conservative therapies cannot protect adjacent teeth or resolve infection, extraction becomes the safest option.
Before any recommendation, clinicians weigh alternatives such as restorative treatment, endodontic therapy, or periodontal care and discuss how extraction will affect long‑term oral health. We explain replacement choices and timing so patients can make informed decisions about function and appearance after healing. Coordination with specialists or medical providers is arranged when complex health factors are present. The goal is predictable care that preserves overall oral wellness.
Evaluation begins with a comprehensive clinical exam, a review of medical history, and focused imaging to assess root anatomy, bone support, and the tooth's relationship to nearby structures. Radiographs and, when appropriate, cone‑beam scans help determine whether a tooth can be removed with simple techniques or will require a surgical approach. We also review current medications, bleeding risks, and any medical conditions that could affect healing. This information guides both the extraction plan and any necessary medical coordination.
Discussion with the patient is an essential part of evaluation; we cover expected outcomes, alternatives, sedation options, and post‑operative care so treatment aligns with the patient's goals. For anxious patients or those with complex medical histories, we outline available comfort measures and collaborate with physicians as needed. A clear, personalized plan reduces uncertainty and supports safer, more comfortable treatment. Follow‑up arrangements are made based on the predicted complexity of the procedure.
A simple extraction is performed on a tooth that is visible in the mouth and can be loosened and removed with forceps after local anesthesia has been administered. These procedures are typically quick and well tolerated, with minimal tissue manipulation and straightforward recovery instructions. Local anesthesia is the primary pain control, and patients usually return to normal activities within a day or two. The clinician will confirm when a follow‑up visit is recommended.
Surgical extraction is used for teeth that are not easily accessible, such as impacted wisdom teeth, broken roots, or teeth with complex root anatomy. This approach may require a small incision in the gum, removal of a bit of bone, and sutures to allow safe removal, and it can involve a slightly longer recovery period. Surgical cases are planned with detailed imaging and may include additional post‑operative monitoring or pain control measures. If a procedure is expected to be surgical, we explain the steps and recovery expectations in advance.
Comfort is a priority and begins with effective local anesthesia to numb the surgical area so patients do not feel pain during the procedure. For patients with dental anxiety or for more complex cases, we offer sedation options to reduce stress and help ensure a smooth experience. Throughout the appointment the team monitors comfort and provides reassurance, adjusting care as needed. Clear communication before the appointment helps determine the right level of sedation and monitoring.
After the extraction, a personalized pain management plan helps keep discomfort at a manageable level while healing begins. We provide instructions on when to take medications, how to minimize swelling, and what signs indicate an expected level of healing. Most patients find post‑operative pain is controllable with the recommended measures and resolves substantially within a few days. If pain is severe or persistent, we ask patients to contact the office promptly for evaluation.
Preparation starts with an accurate medical history and a list of current medications so the team can identify any bleeding risks, drug interactions, or conditions that require special planning. If you are scheduled for sedation, follow fasting instructions and arrange for a responsible adult to drive you home after the appointment. Notify the office about any recent illnesses, changes in medications, or cardiac conditions so we can coordinate with your physician when necessary. Bring any relevant medical documentation and a list of questions to your visit.
Follow pre‑operative instructions provided by the office, which may include guidance on usual medications, alcohol and tobacco use, and the timing of arrival. Comfortable clothing and avoidance of strong fragrances can improve the comfort of patients sensitive to smells. If you have concerns about anxiety, we will discuss relaxation or sedation options ahead of time to ensure you feel supported. Clear preparation helps the appointment proceed safely and efficiently.
During the first 24 to 48 hours you can expect some bleeding, swelling, and mild to moderate discomfort as the body forms a blood clot and begins healing the socket. Keeping gentle pressure on the gauze, resting, and using cold packs intermittently can help control bleeding and swelling in the immediate post‑operative period. Follow the provided medication instructions to keep pain at a tolerable level, and avoid activities that could dislodge the clot. Most patients notice steady improvement after the initial two days.
Over the first week soft tissues will continue to heal and swelling will gradually subside, with full soft‑tissue closure taking several weeks in many cases. Maintain oral hygiene by gently cleaning the surrounding teeth and using warm saltwater rinses after 24 hours, taking care not to disturb the extraction site. If sutures were placed, your clinician will advise whether they will be removed or will dissolve on their own. We schedule follow‑up as needed to monitor healing and plan any future restorative steps.
Protecting the forming blood clot is the most important step to reduce the risk of dry socket; avoid vigorous rinsing, spitting, use of straws, and smoking for several days after the extraction. Follow all post‑operative instructions about gauze changes, activity restrictions, and medication timing to support predictable healing. Maintain gentle oral hygiene around the extraction site and take any prescribed antibiotics as directed to lower infection risk. Good hydration and a soft diet in the early days also support recovery.
Be mindful of signs that may indicate a complication, such as increasing pain after the first few days, a bad taste or odor in the mouth, or prolonged heavy bleeding, and contact the office promptly if these occur. Early evaluation allows the team to treat issues like dry socket or infection quickly and minimize discomfort. We will explain preventive steps specific to your case and schedule follow‑up when the procedure warrants closer monitoring. Timely communication helps ensure the best possible outcome.
You should call the office if you experience persistent heavy bleeding that soaks through gauze after a few hours, a fever above 101°F, increasing or uncontrolled pain despite medication, or sudden and severe swelling. Other reasons to contact the practice include numbness that does not resolve, signs of infection such as spreading redness or a foul taste, or if stitches come loose unexpectedly. If you have been given emergency contact instructions, use them for after‑hours concerns that require immediate attention. Prompt communication allows us to evaluate symptoms and advise appropriate next steps.
For routine follow‑up or questions about diet, medication, and activity restrictions, contacting the office during regular hours is appropriate and helps us determine whether an in‑person exam is needed. We encourage patients to report any unusual symptoms rather than waiting, since early intervention can prevent more serious problems. Keep your follow‑up appointment so the clinician can confirm healing and address any emerging needs. Clear post‑op communication supports safe recovery.
Replacement options commonly include removable dentures, fixed dental bridges, and dental implants, each with distinct benefits related to stability, appearance, and maintenance. Removable dentures can restore immediate function in some cases, while fixed bridges provide a stable restoration when adjacent teeth are healthy. Dental implants offer the most natural feel and help preserve jawbone by replacing the tooth root, but they require sufficient bone volume and a staged treatment plan. The best choice depends on the location of the missing tooth, oral health, and the patient's functional and aesthetic goals.
Timing for replacement varies with the procedure and healing; some options can be initiated soon after extraction, while implants often require a period of healing or grafting to ensure adequate bone support. We evaluate bone levels and overall health to recommend a restorative timeline that balances prompt function with optimal long‑term outcomes. Discussion of risks, benefits, and maintenance needs for each option helps patients select a solution that fits their lifestyle. Follow‑up planning ensures the replacement integrates well with ongoing oral care.
At Horizon Palms Family Dentistry in Lake Worth, our team combines clinical experience with individualized planning to deliver predictable, safe extraction care tailored to each patient. We use modern imaging and techniques to minimize tissue trauma and coordinate with specialists or medical providers when cases require advanced surgical support. Comfort measures, clear communication about what to expect, and thorough pre‑ and post‑operative instructions are central to our approach. This structured process helps patients heal efficiently and preserve long‑term oral health.
We prioritize patient education and shared decision making so each person understands alternatives, procedural steps, and restorative options after extraction. Our clinicians stay current with best practices and emphasize conservative care when appropriate, recommending removal only when it is the most responsible choice for oral health. Follow‑up care and timely access to the team for concerns are part of the treatment commitment. The result is care focused on safety, function, and predictable outcomes.

