
Our Office
5909 South Congress Ave
Lake Worth, FL 33462
Existing Patients: (561) 967-6453
New Patients: (561) 203-0359
Emergency: (754) 800-1949
Fax: (561) 431-5866
Visit Us Online
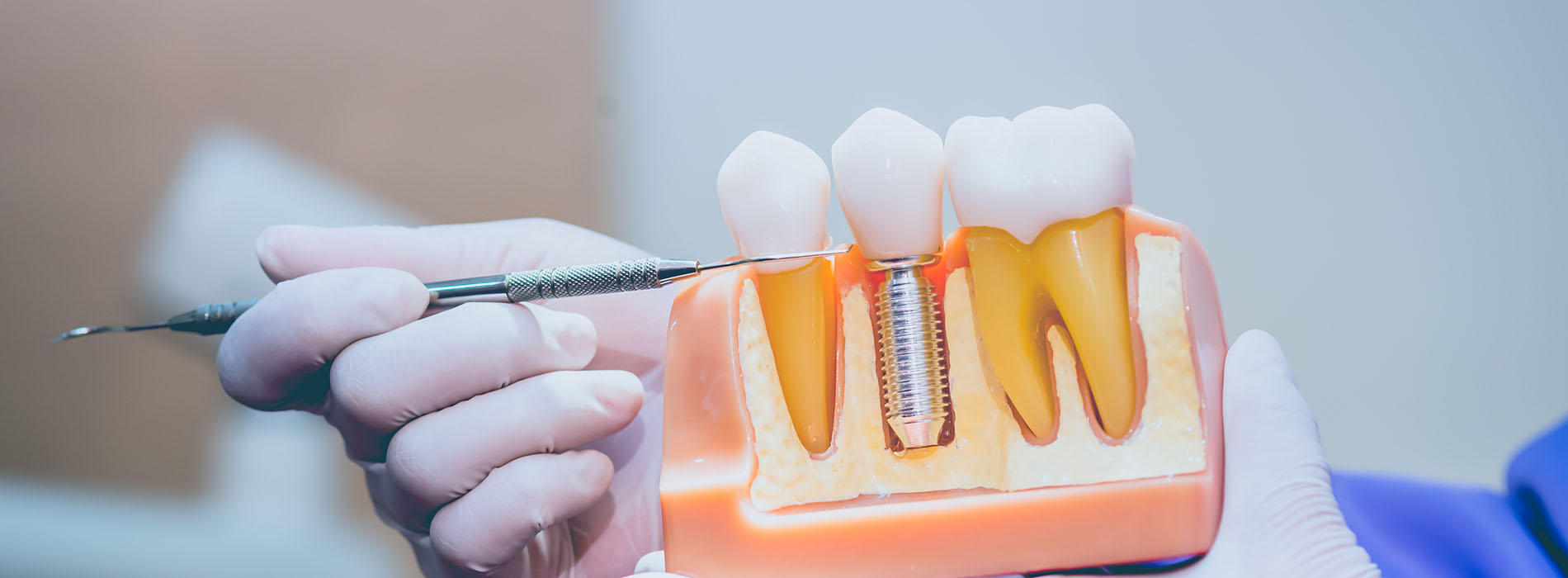
Implant restorations replace missing teeth with prosthetics anchored to titanium posts surgically placed in the jaw. Unlike removable dentures that sit on the gums, implant-supported restorations connect to a stable foundation in the bone, which helps restore chewing function and facial support. The end result looks and behaves much more like a natural tooth because the prosthetic is supported from within the jaw rather than simply resting on top of it.
Modern implant restorations rely on a biologic process called osseointegration, where the bone gradually bonds to the surface of the implant. This fusion creates a solid, long-term anchor for crowns, bridges, or overdentures. Because implants integrate with the jaw, they also help preserve surrounding bone and prevent the gradual bone loss that commonly follows tooth extraction.
For many patients, implant restorations offer a durable, comfortable, and aesthetic option for replacing one or several missing teeth. They can restore bite force, improve speech, and provide a natural appearance that supports confidence in everyday life. Implant restorations are a restorative solution rather than a cosmetic quick fix; they address both function and form.
Implant restorations are an option for a wide range of patients who have lost one or more teeth. Good candidates generally have healthy gums and adequate jawbone to support the implant. When bone volume is insufficient, grafting procedures or alternative implant placements can often be used to create a stable foundation. A thorough clinical exam and imaging help determine the most appropriate approach for each patient.
General health is also a consideration. Conditions that affect healing—such as uncontrolled diabetes, certain autoimmune disorders, or heavy tobacco use—can influence success rates and may require medical collaboration or lifestyle adjustments. That said, many patients with well-managed systemic conditions can move forward with implants after consultation with their medical providers.
Age by itself is rarely a limiting factor; instead, bone quality, oral health, and overall medical status matter most. Whether replacing a single tooth, multiple adjacent teeth, or an entire arch, implant restorations can be customized to meet individual needs and long-term goals for oral function and appearance.
The implant restoration journey begins with careful planning. Diagnostic records, including digital X-rays or CBCT scans, are used to evaluate bone structure, nerve position, and the relationship between teeth and jaws. Treatment planning can include choosing the right implant size, planning for any needed bone grafting, and deciding whether a temporary prosthesis will be placed during healing.
Placement of the implant post is a minor oral surgery typically performed under local anesthesia. After placement, a healing period allows the implant to integrate with the bone. This healing time varies by patient and location in the mouth but typically ranges from a few weeks to several months. During this phase, patients receive instructions to protect the site and maintain excellent oral hygiene.
Once the implant has integrated, an abutment is attached to support the final restoration. The laboratory-crafted crown, bridge, or overdenture is then secured to the abutment and adjusted for fit, color, and bite. The result is a restoration that is shaped and shaded to blend with surrounding teeth while restoring proper function.
Implant prosthetics are flexible and can be designed to match the needs of each patient. A single implant often supports a single crown, offering a lifelike replacement for an individual tooth without relying on neighboring teeth for support. For areas with multiple missing teeth, implant-supported bridges can replace several teeth in a row with fewer implants than the number of teeth replaced.
When many or all teeth in an arch are missing, implant-supported dentures or fixed hybrid prostheses provide robust solutions that significantly improve chewing ability and stability compared with traditional removable dentures. These designs can be either removable by the patient for cleaning or fixed in place and only removable by a clinician, depending on the chosen system and clinical goals.
Materials used for implant restorations vary according to strength and aesthetic requirements. Ceramic crowns and custom-milled frameworks are common choices because they provide both durability and a natural appearance. During treatment planning, clinicians balance longevity, esthetics, and the specific functional demands of each tooth position.
Proper home care and routine professional checkups are essential to the longevity of implant restorations. Daily brushing, interdental cleaning, and attention to the tissues around the implant help prevent inflammation and protect the supporting bone. Patients are instructed in techniques and tools that make cleaning around implants effective and comfortable.
Regular dental visits allow clinicians to monitor integration, restorative fit, and the health of surrounding gum tissues. Periodic imaging and clinical exams detect early signs of complications—such as peri-implant mucositis or bone changes—so they can be managed promptly. Early intervention typically improves outcomes and minimizes the need for more extensive treatment.
While implant restorations are engineered for durability, they require ongoing care like any dental work. Avoiding habits that place excessive force on restorations—such as chewing on hard objects or teeth grinding—helps preserve the prosthetic and supporting structures. When maintenance is followed and oral health is preserved, implant restorations can provide many years of reliable function.
Implant restorations are a predictable way to replace missing teeth with results that restore function, preserve bone, and produce a natural appearance. At Horizon Palms Family Dentistry in Lake Worth, our care team combines modern planning tools and restorative expertise to guide patients through every stage of implant treatment. Contact us to learn more about whether implant restorations are the right solution for your smile.
Implant restorations replace missing teeth with prosthetic teeth that attach to titanium posts surgically placed in the jaw. These posts act as artificial tooth roots and provide a stable foundation for crowns, bridges, or overdentures. Over time, bone bonds to the implant surface through a process called osseointegration, creating long-term stability.
Because the prosthetic is anchored in bone rather than resting on the gums, implant restorations restore chewing function and help preserve facial support. They can improve speech and chewing comfort while providing an appearance that closely matches natural teeth. Implant restorations are designed to address both function and form rather than serving as a short-term cosmetic fix.
Candidates typically have healthy gums and sufficient jawbone to support an implant. A clinical exam and imaging are used to assess bone volume, tooth position, and the relationship of nearby nerves and sinuses. General health factors that affect healing, such as uncontrolled diabetes or heavy tobacco use, may require medical coordination or lifestyle changes before treatment.
When bone volume is insufficient, grafting procedures or alternative implant placements can often create a stable foundation for restoration. Your dental team will review possible approaches, including immediate placement and staged protocols, based on your anatomy and goals. A personalized treatment plan identifies the best timing for surgery, provisional restorations, and final prosthetics to optimize outcomes.
Osseointegration is the biologic process in which bone grows and bonds to the surface of an implant. This fusion creates the rigid connection needed for the implant to support a crown, bridge, or denture under normal chewing forces. Successful osseointegration is the foundation of long-term implant stability and function.
The timeframe for osseointegration varies by patient and location in the mouth, commonly ranging from several weeks to a few months. Factors such as bone density, surgical technique, and systemic health influence the speed and quality of integration. Good oral hygiene and adherence to post-operative instructions help promote predictable healing and reduce the risk of complications.
The process begins with diagnostic planning that includes digital X-rays or CBCT scans to evaluate anatomy and plan implant placement. Surgical placement of the implant post is typically a minor oral surgery performed under local anesthesia, and healing time for integration commonly takes weeks to months. Temporary restorations may be used during healing to maintain appearance and function when appropriate.
After integration, an abutment is attached and impressions or digital scans are used to fabricate the final crown, bridge, or overdenture. The timing for final restoration depends on healing, soft tissue maturation, and laboratory work, all of which are coordinated to achieve an accurate fit and natural appearance. Individual treatment timelines vary, and your clinician will outline milestones and expected intervals during planning.
Single implants commonly support individual crowns that replace one missing tooth without altering adjacent teeth. For multiple missing teeth, implant-supported bridges can span several spaces with fewer implants than teeth replaced, preserving surrounding natural dentition. When an entire arch is missing, implant-supported dentures or fixed hybrid prostheses restore function and stability far better than traditional removable dentures.
These prosthetics can be designed as removable overdentures that the patient can take out for cleaning or as fixed restorations that are removed only by a clinician. Material choices range from ceramic crowns and custom-milled frameworks to zirconia components, and selections are made based on strength and esthetic needs. Your clinician will recommend the option that best balances durability, appearance, and the functional demands of each tooth position.
Daily oral hygiene is essential; brush twice a day and use interdental brushes or floss designed for implants to clean around the abutment and prosthetic surfaces. Maintaining healthy gum tissue around the implant helps prevent inflammation and protect the supporting bone. Avoiding habits that place excessive force on restorations, such as chewing hard objects, reduces the risk of mechanical damage.
Your dental team will demonstrate effective cleaning techniques and may recommend specific tools to reach areas around the implant. If you have bruxism or grinding, a night guard can reduce harmful forces that accelerate wear and component loosening. Consistent home care combined with regular professional maintenance supports long-term success.
Potential complications include peri-implant mucositis, peri-implantitis with bone loss, infection, and mechanical issues such as screw loosening or prosthetic fracture. Early signs like redness, swelling, bleeding on probing, or changes in fit should prompt evaluation by your dentist. Timely detection increases the likelihood of conservative management and better outcomes.
Management strategies range from professional cleaning and non-surgical therapy to surgical intervention for regenerative procedures when indicated. Mechanical problems are often resolved by repairing or replacing components, while persistent inflammation may require specialist care and collaboration with medical providers. Long-term monitoring and adherence to maintenance recommendations help minimize the risk of serious complications.
Yes, full-arch replacement can be achieved with implant-supported dentures or fixed hybrid prostheses that restore both appearance and chewing function. These solutions use strategically placed implants to support a prosthetic arch that is far more stable than conventional dentures. Treatment can be planned to minimize the number of implants while optimizing support and distribution of forces.
Choices include removable overdentures that snap onto implants for patient-directed cleaning or fixed prostheses that are secured to implants for a permanent feel. Clinical factors such as bone quantity, ridge anatomy, and patient hygiene capability guide the selection between removable and fixed designs. A comprehensive evaluation determines the most predictable approach for full-arch restoration.
Ceramic materials such as lithium disilicate and zirconia are commonly used for crowns and frameworks because they combine strength with a natural appearance. Titanium is the standard material for implant posts due to its proven biocompatibility and mechanical properties. Custom-milled frameworks and high-strength ceramics allow clinicians to match color, shape, and translucency to neighboring teeth.
Material selection depends on the location in the mouth, bite forces, esthetic priorities, and restorative design. For posterior teeth, strength and wear resistance may take precedence, while anterior restorations often emphasize translucency and color matching. Your clinician will discuss the advantages and limitations of different materials when designing your restoration.
Treatment begins with a thorough examination, digital imaging, and, when appropriate, CBCT scans to map bone anatomy and identify vital structures such as nerves and sinuses. These diagnostic records support precise implant selection, surgical guides, and a comprehensive plan that anticipates prosthetic contours and esthetic outcomes. Collaborative planning among the clinician, laboratory technicians, and the patient helps align expectations and technical steps.
Surgical placement, provisional restorations, and final prosthetic fabrication are scheduled to allow predictable healing and accurate fit, with periodic reviews during each phase. The practice coordinates laboratory work, post-surgical care, and long-term maintenance to protect the restoration and supporting tissues. If needed, the team works with medical providers to address systemic factors that could affect healing and long-term success.

