Our Office
5909 South Congress Ave
Lake Worth, FL 33462
Existing Patients: (561) 967-6453
New Patients: (561) 203-0359
Emergency: (754) 800-1949
Fax: (561) 431-5866
Visit Us Online
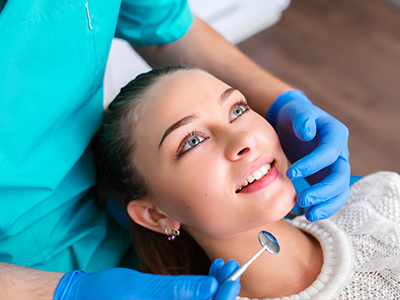
Nearly half of adults over the age of 30 show signs of periodontal (gum) disease, making it one of the most common threats to long-term tooth retention. The condition begins quietly for many people and can advance without obvious pain, which is why early recognition and consistent care are so important. At Horizon Palms Family Dentistry, we focus on clear explanations and practical treatment plans so patients understand both the risks and the realistic paths to recovery.
Gum disease is the umbrella term for inflammation and infection of the tissues that support your teeth. It originates when dental plaque — a biofilm of bacteria that forms on teeth — accumulates and hardens into calculus (tartar). That bacterial load triggers the body’s immune response, which over time damages the soft tissue and the bone that hold teeth in place.
Because early stages can be subtle, many people assume swollen or easily bleeding gums are temporary or harmless. In reality, those signs are signals that the tissues are under stress. Left unchecked, the inflammatory process can progress from treatable irritation to progressive tissue breakdown and tooth mobility.
Recognizing periodontal disease as a biological process — one that responds to both professional care and everyday habits — helps patients take meaningful steps to preserve their oral health. Regular monitoring, combined with targeted treatment when necessary, puts control back in the patient’s hands.
Gum health is not only about keeping teeth in place; it also plays a role in overall well-being. Research has identified connections between chronic periodontal inflammation and broader health concerns, including cardiovascular disease, diabetes management, and respiratory health. While these links are complex and still being studied, they underline the importance of managing gum disease proactively.
Good periodontal care reduces local infection and inflammation, which can make daily life more comfortable and reduce the likelihood of more involved procedures later on. Preventing advanced disease also protects the function of your bite and the long-term stability of restorative work such as crowns and implants.
At Horizon Palms Family Dentistry, we emphasize prevention and early intervention so that treatment focuses on preserving tissue rather than replacing it. Helping patients understand these connections encourages consistent home care and timely professional follow-up.
Gingivitis is the initial, reversible stage of gum disease. It shows up as redness, swelling, and bleeding during brushing or flossing. Because it typically doesn’t cause severe pain, gingivitis is often overlooked until a routine exam or cleaning reveals the problem. Identifying gingivitis early can prevent irreversible damage.
Treatment for gingivitis centers on removing the causes of inflammation: professional cleaning to eliminate plaque and tartar combined with improved at-home oral hygiene. Small adjustments — consistent brushing technique, daily interdental cleaning, and regular dental visits — often restore healthy gum tissue without the need for more invasive procedures.
Monitoring is an important part of care after gingivitis has been treated. Periodic reassessment helps confirm that the tissue has healed and that patients have adopted sustainable habits to keep plaque under control moving forward.

If inflammation beneath the gumline persists, gingivitis can evolve into periodontitis — a destructive condition that damages the connective tissues and bone supporting teeth. This phase is characterized by the development of periodontal pockets, gum recession, and, ultimately, loosening of teeth. The process is gradual, but its consequences can be permanent if not addressed.
Treatment in this stage is aimed at stopping tissue loss and, where possible, restoring lost support. That may involve a combination of deeper cleaning procedures, targeted antimicrobial therapies, and, in select cases, surgical interventions to repair or regenerate damaged tissues. The earlier periodontitis is identified, the more options there are to limit its effects.
Managing periodontitis also requires attention to contributing factors such as tobacco use, systemic health conditions, and habits that affect plaque accumulation. A comprehensive plan addresses both local infection and those broader influences to improve the likelihood of a durable outcome.
Contemporary periodontal care blends clinically proven techniques with patient-centered planning. We use diagnostic assessments to measure pocket depths, evaluate bone levels, and identify active areas of inflammation. From that evaluation, a customized plan is created that prioritizes the least invasive effective option for each individual.
Non-surgical therapies remain an essential first step for many patients: precise scaling and root planing, antimicrobial applications, and a focused hygiene regimen can arrest disease in a large number of cases. When indicated, adjunctive measures — such as localized antimicrobials or systemic medications — can help reduce bacterial burden and promote healing.
When regenerative or reconstructive needs arise, modern surgical techniques, biologic materials, and, where appropriate, laser-assisted therapy provide additional tools to restore tissue contours and function. Our goal is to combine science, experience, and patient preferences to reach predictable, long-lasting results.
Choosing the right treatment depends on disease stage, the depth of periodontal pockets, bone support, and overall health. A thorough periodontal examination guides the recommendation, and we discuss risks, expected benefits, and maintenance requirements so patients can make informed decisions. Open communication and realistic expectations are core to successful care.
Initial therapy commonly involves comprehensive scaling and root planing to remove bacterial deposits and smooth root surfaces so tissues can reattach. This phase is often followed by a short course of targeted antimicrobial therapy when indicated, and frequent re-evaluations to confirm improvement in pocket depths and tissue health.
When pockets remain deep or structural damage is significant, surgical approaches may be recommended to gain access for cleaning, reduce pocket depth, or reconstruct lost bone and connective tissue. Surgery is intended to improve long-term maintenance and reduce the risk of future tooth loss, not merely to treat symptoms temporarily.
For many patients, non-surgical care provides an effective path back to periodontal health. Scaling and root planing remove plaque and tartar below the gumline and smooth exposed root surfaces to discourage future buildup. This mechanical approach directly reduces the bacterial triggers of inflammation.
Adjunctive options may include placing localized antimicrobials beneath the gums or recommending systemic agents in cases where the overall infection burden warrants additional support. These measures are chosen based on clinical findings and tailored to each patient’s medical history and treatment goals.
Success with non-surgical therapy depends heavily on daily oral hygiene and regular maintenance visits. A structured recall schedule helps ensure early detection if disease activity returns and reinforces the habits that support long-term stability.
If initial conservative care does not adequately reduce pocket depths or resolve inflammation, surgical options may be discussed as the next step in the treatment continuum.
Surgery becomes a consideration when disease has progressed to the point where pockets are too deep for non-surgical cleaning or where tissue and bone loss threaten tooth support. The aim of periodontal surgery is to access and remove persistent bacterial deposits, reshape defects, and create anatomy that patients can keep clean more easily.
Periodontal procedures may include flap surgery to reduce pocket depth, guided tissue regeneration to encourage new attachment, and bone grafting when bone volume needs restoration. In many cases these procedures are performed with the goal of preserving natural teeth and improving the foundation for future restorative work.
Minimally invasive techniques and advanced instruments, including lasers in select applications, can reduce discomfort and speed recovery for some patients. A careful decision-making process determines which surgical approach best balances treatment goals, predictability, and patient comfort.
The primary surgical goals are to eliminate disease-causing bacteria, stabilize or rebuild the supporting structures, and create a healthier environment that supports long-term maintenance.
Remove sub-gingival bacteria and deposits from root surfaces
Limit further bone loss and, when possible, restore lost hard tissue
Reduce pocket depth to make daily cleaning more effective and reduce recurrence risk

Successful periodontal care is a partnership between clinician and patient: clinical interventions create the opportunity for healing, and consistent home care preserves those gains. Our clinicians focus on clear explanations, measurable goals, and personalized maintenance strategies to help patients keep their gums healthy for years to come.
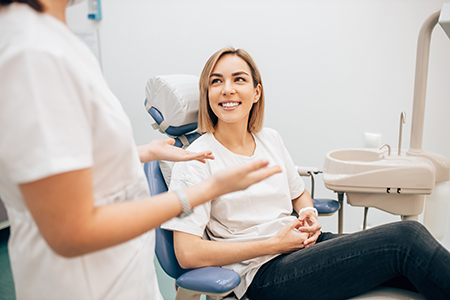
We offer modern, evidence-based periodontal treatment options in a calm, patient-centered setting. If you have noticed bleeding, swelling, persistent bad breath, or loosening teeth, evaluation and early action can make a meaningful difference in outcomes. Contact us to learn more about how we can help you protect and restore your gum health.
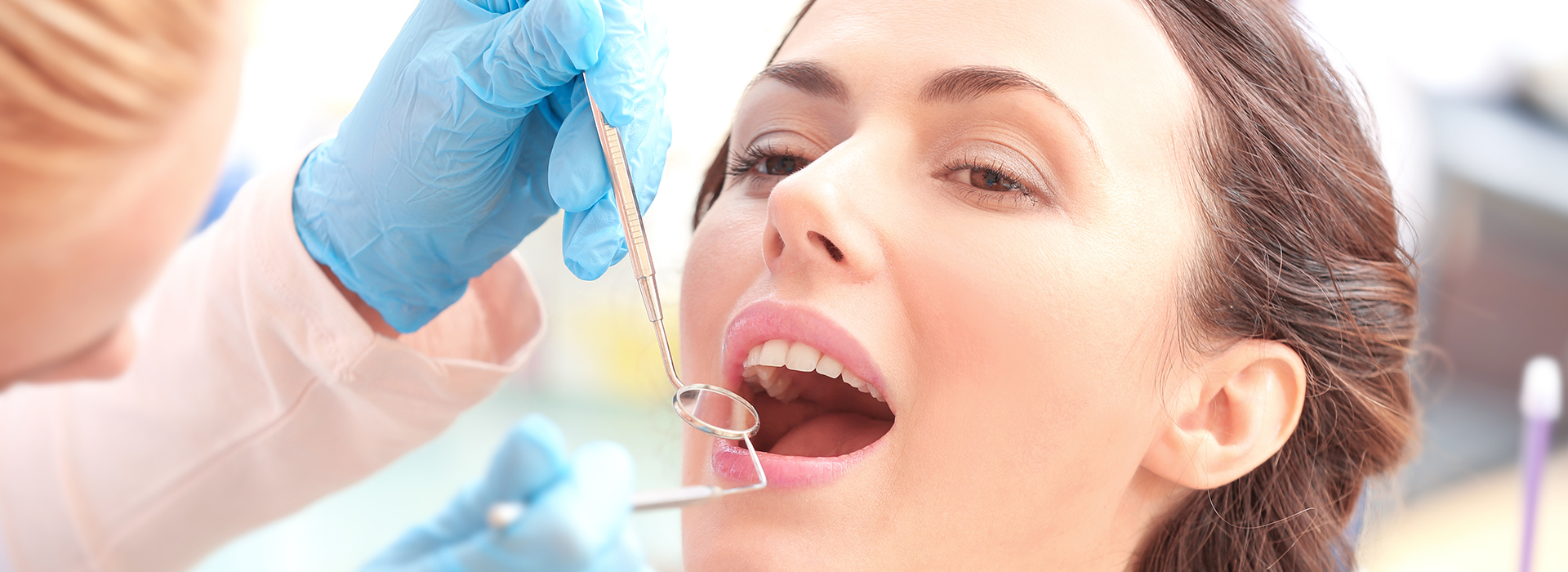
Periodontal disease is an infection and inflammation of the tissues that support the teeth, including the gums, periodontal ligament and underlying bone. It develops when dental plaque, a sticky bacterial film, accumulates on tooth surfaces and hardens into calculus beneath the gumline. That bacterial challenge triggers the body’s immune response, and repeated inflammation gradually damages soft tissue and bone.
Because early stages can be painless, many people do not notice the problem until tissue breakdown has progressed. Left unchecked, the condition can lead to periodontal pockets, gum recession and tooth mobility. Early recognition and treatment improve the chances of preserving natural teeth and preventing more invasive procedures.
Common early signs include gums that bleed during brushing or flossing, redness, swelling and persistent bad breath or a bad taste in the mouth. You may also notice gums that feel tender or pull away from teeth, creating the appearance of longer teeth. These symptoms often appear before pain and should prompt a professional evaluation.
Because many signs are subtle, routine dental exams and cleanings are important for catching disease at an early, reversible stage. If you notice any changes in your gums or bite, document when symptoms started and share that information during your visit. Early action typically requires less invasive treatment and better long-term outcomes.
Gingivitis is the initial, reversible stage of gum disease characterized by inflammation of the gum tissue without loss of bone or connective tissue. It usually shows as redness, swelling and bleeding but does not yet involve the deeper attachment structures around the tooth. With appropriate professional cleaning and improved home care, gingivitis commonly resolves.
Periodontitis occurs when inflammation extends below the gumline and destroys the connective tissues and bone that support teeth. This stage produces periodontal pockets, progressive attachment loss and sometimes irreversible damage that requires deeper therapy. Managing periodontitis often involves a combination of professional treatment and ongoing maintenance to control infection and prevent further loss.
Diagnosis begins with a comprehensive periodontal exam that includes measuring pocket depths around each tooth, checking for bleeding on probing and assessing gum recession. Dental radiographs are used to evaluate bone levels and identify areas of bone loss that may not be visible clinically. The clinician also reviews your medical history and risk factors to understand the full picture that may influence treatment choices.
Charting and photographic documentation help track disease activity over time and measure response to therapy. Periodic reassessment after initial treatment determines whether the plan is working or if additional steps are needed. Clear communication about findings and measurable goals helps patients participate in their care.
Non-surgical therapy typically begins with scaling and root planing, a careful cleaning that removes plaque and calculus from below the gumline and smooths root surfaces to encourage reattachment of the gum to the tooth. This mechanical approach reduces the bacterial load and the inflammation driving tissue destruction. Many patients respond well to this level of care when combined with improved oral hygiene at home.
Adjunctive therapies can include localized antimicrobial agents placed into periodontal pockets and, in select cases, systemic medications to address a high infection burden. Success depends on adherence to daily oral hygiene and a structured maintenance schedule. If pockets do not respond adequately, clinicians discuss further options, including surgical approaches.
Surgery is considered when pockets remain deep despite non-surgical therapy or when anatomical defects and bone loss threaten tooth support and oral function. The goal of surgery is to gain access for thorough cleaning, reduce pocket depth, and where possible restore or regenerate lost bone and connective tissue. Indications are based on clinical measurements, radiographic findings and the patient’s overall health.
Common surgical procedures include flap surgery to access and clean root surfaces, guided tissue regeneration to encourage new attachment, and bone grafting to rebuild lost hard tissue. Minimally invasive techniques and, in select cases, laser-assisted therapies can reduce discomfort and speed recovery. The emphasis is always on choosing the approach that best balances predictability, long-term stability and patient comfort.
Maintaining gum health is an ongoing partnership between patient and clinician, centered on consistent daily oral hygiene and scheduled professional care. Brushing twice daily with a fluoride toothpaste, cleaning between teeth daily with floss or interdental brushes and following personalized home-care instructions are essential. Periodontal maintenance visits at regular intervals allow the clinician to remove new deposits, monitor pocket depths and reinforce preventive habits.
Addressing modifiable risk factors improves long-term success: quitting tobacco use, managing diabetes and reviewing medications that affect oral tissues are important steps. Open communication about lifestyle changes and symptoms helps the care team adjust the maintenance plan as needed to protect your periodontal health. Consistency is the single most important factor in preventing recurrence.
Research has identified associations between chronic periodontal inflammation and systemic conditions such as cardiovascular disease, diabetes control and respiratory health. While these relationships are complex and not fully understood, persistent oral inflammation contributes to the body’s overall inflammatory burden. Reducing periodontal infection and inflammation can therefore be an important part of a broader health strategy.
Managing gum disease can improve comfort and oral function while potentially supporting better outcomes for certain medical conditions. Clinicians often coordinate care with physicians when systemic factors influence periodontal health, and patients are encouraged to inform their medical providers about significant periodontal concerns. Preventive care and early intervention remain practical ways to protect both oral and general health.
Several factors increase the risk of periodontal disease, including tobacco use, uncontrolled diabetes, advancing age and a family history of aggressive disease. Poor oral hygiene, certain medications that reduce saliva flow or cause gum overgrowth, and restorative work that traps plaque can also raise risk. Stress, hormonal changes and systemic illnesses further influence susceptibility.
Because some risk factors are modifiable, targeted interventions can reduce long-term risk: smoking cessation, improved glucose control and meticulous plaque control are examples. Regular dental evaluations help identify early signs in patients with known risks so treatment can begin before irreversible damage occurs. A personalized approach to risk reduction improves outcomes for most patients.
At Horizon Palms Family Dentistry in Lake Worth, a periodontal visit begins with a focused review of your medical and dental history followed by a thorough clinical exam that measures pocket depths, assesses bleeding and evaluates gum and bone support. Radiographs may be taken to visualize bone levels and identify areas of concern not visible during the clinical exam. The clinician will explain findings in clear terms and answer your questions so you understand the condition and available options.
A customized treatment plan is then proposed with an emphasis on the least invasive effective therapies and measurable goals for improvement. Our team discusses home-care strategies and schedules follow-up or maintenance visits to monitor healing and prevent recurrence. Comfort measures and clear communication are central to care so patients feel informed and supported every step of the way.

